Easy Methods To Combat Pes Planus

Most people have a gap under the arch of their foot when they are in a standing position. The arch, the inner part of the foot is slightly raised off the ground. People with flat feet or fallen arches either have no arch, or it is very low. The feet of people with flat feet may roll over to the inner side when they are standing or walking, and the feet may point outwards as a result.
Causes
A fallen arch occurs because one of the main structures that support the arch has broken or torn. Usually it occurs without trauma, although a small injury associated with the onset of the pain is often recalled, it is sometimes difficult to determine whether the injury was clearly big enough to permanently injure the leg. I suspect that even before the symptoms that the structure that broke was weakening and the injury was simply the ?needle that broke the camels back?. The structure that is most commonly torn is the posterior tibial tendon. This tendon is attached to a muscle on the inside of the back of the ankle, and runs along the medial malleolus, the bony prominence on the inside of the ankle, to attach to a bone in the arch called the navicular bone. It usually begins to weaken and stretch along the back of the medial malleolus. It often begins as a swelling and the arch flattens over the next several weeks to months. As the arch flattens, other structures that support the arch begin to stretch and tear. The bones along the outside of the ankle begin to crush together, causing pain and swelling in this are, and the toes may tilt to the outside as the arch collapses. It is not known why this process begins. It is often associated with diabetes and rheumatoid arthritis and other inflammatory diseases. It also is more common as a person enters the fifty to seventy year age range. ?Fallen arches? are much more common in people who are already flat footed.
Symptoms
Most patients who suffer from flat feet or fallen arches often do not complain of any symptoms whatsoever. However, on some occasions, patients may find that their feet are fatigued fairly easily and following activity on long periods of standing may have a painful foot or arch. On occasions, swelling may be seen on the inner aspect of the foot and performing certain movements may be painful and difficult. Some patients who have flat feet may find that their feet tend to roll in (over-pronate) a lot more when they walk and run. As a result, they may experience damage to the ankle joint and the Achilles tendon, as well as excessive shoe wear.
Diagnosis
You can always give yourself the ?wet test? described above to see whether you have flat feet. Most people who do not notice their flat feet or have no pain associated with them do not think to see a foot doctor. Flat feet can lead to additional problems such as stiffness or pain, however, especially if the condition appears out of nowhere. If you think you may have flat feet, you should seek medical attention to ensure there are no additional issues to worry about. Your doctor will be able to diagnose you with a number of tests. For example, he or she may have you walk around, stand still, or stand on your tiptoes while you are being examined. Your doctor may also examine your foot?s shape and functionality. It?s important to let your foot doctor know about your medical and family history. In some cases, your doctor may order imaging tests such as x-rays or an MRI (magnetic resonance imaging) to determine a cause of your flat foot. If tarsal coalition is suspected in children, a CT scan is often ordered.
arch supports for high arches
Non Surgical Treatment
Normally, flat feet disappear by age six as the feet become less flexible and the arches develop. Only about 1 or 2 out of every 10 children will continue to have flat feet into adulthood. For children who do not develop an arch, treatment is not recommended unless the foot is stiff or painful. Shoe inserts won?t help your child develop an arch, and may cause more problems than the flat feet themselves. However, certain forms of flat feet may need to be treated differently. For instance, a child may have tightness of the heel cord (Achilles tendon) that limits the motion of his foot. This tightness can result in a flat foot, but it usually can be treated with special stretching exercises to lengthen the heel cord. Rarely, a child will have truly rigid flat feet, a condition that can cause problems.
Surgical Treatment

Generally one of the following procedures is used to surgically repair a flat foot or fallen arch. Arthrodesis. One or more of your bones in the foot or ankle are fused together. Osteotomy. Correcting alignment by cutting and reshaping a bone. Excision. Removing a bone or a bone spur. Synovectomy. Cleaning the sheath that covers the tendon. Tendon transfer. Using a piece of one tendon to lengthen or replace another. Arthroereisis. placing a small device in the subtalar joint to limit motion. For most people, treatment is successful, regardless of the cause, although the cause does does play a major role in determining your prognosis. Some causes do not need treatment, while others require a surgical fix.
After Care
Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.
All You Will Need To Understand About Heel Serious Pain
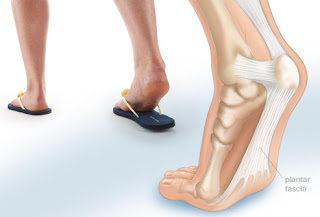
Heel pain is a very common foot complaint and may involve injury to the bone, fat pad, ligaments, tendons or muscles. Heel pain can also be referred by a pinched nerve in your lower back. It is important to have your heel pain thoroughly assessed to ensure an accurate diagnosis and subsequent treatment. Anyone can suffer from heel pain, but certain groups seem to be at increased risk, including middle aged men and women, active people eg running sports, people who are very overweight, children aged between 8 and 13 years, pregnant women, people who stand for long periods of time.
Causes
Here are a few in-depth explanations of heel pain causes and potential remedies for those that are afflicted Plantar Fascitis, One of the most well-known causes of heel pain, plantar fascitis occurs when the thick tissue along the arch of the foot becomes tight and inflamed. The foot itself can feel cramped when this tissue is inflamed, causing the afflicted person to feel as if they have a muscle cramp that flexing the foot doesn?t seem to alleviate. Plantar fascitis is most common among men over the age of 40. Warning Signs, The first steps in the morning are extremely painful. Pain flares up after activities like stair or steep hill climbing. Pain continues to occur regardless of the type of shoes or lack of shoes worn.
Symptoms
Pain typically comes on gradually, with no injury to the affected area. It is frequently triggered by wearing a flat shoe, such as flip-flop sandals. Flat footwear may stretch the plantar fascia to such an extent that the area becomes swollen (inflamed). In most cases, the pain is under the foot, toward the front of the heel. Post-static dyskinesia (pain after rest) symptoms tend to be worse just after getting out of bed in the morning, and after a period of rest during the day. After a bit of activity symptoms often improve a bit. However, they may worsen again toward the end of the day.
Diagnosis
In most cases, your GP or a podiatrist (a specialist in foot problems and foot care) should be able to diagnose the cause of your heel pain by asking about your symptoms and medical history, examining your heel and foot.
Non Surgical Treatment
Treatments to add to your stretching program include wearing good-quality shoes, icing the painful area, and massaging the arch. Do not walk barefoot; walk in shoes with good heel and arch supports such as high-quality walking or running shoes. Keep a pair of shoes next to your bed so you can put them on before taking your first step. Your doctor may recommend that you wear an additional arch support or a heel cup in the shoes. Icing your foot can help relieve pain. Rub a frozen bottle of water or an ice cup over the tender areas for five minutes two times each day. Massage your foot by rolling a tennis, golf ball, or baseball along your sole and heel. This friction massage can help break up adhesions and stretch the plantar fascia. Do this for five minutes two times each day. If you are a runner or just started a walking or running program, evaluate your training for errors such as warming up improperly, increasing mileage too quickly, running hills excessively, running on surfaces that are too hard, or wearing broken down shoes. Adjusting your training program can help relieve your pain. While recovering from heel pain, walk or jog in a pool or crosstrain by biking and swimming. These activities maintain your cardiovascular fitness without stressing your heel cord or plantar fascia. Heel pain takes time to go away. Be patient and remember that no treatment is a substitute for STRETCHING!
Surgical Treatment
Surgery to correct heel pain is generally only recommended if orthotic treatment has failed. There are some exceptions to this course of treatment and it is up to you and your doctor to determine the most appropriate course of treatment. Following surgical treatment to correct heel pain the patient will generally have to continue the use of orthotics. The surgery does not correct the cause of the heel pain. The surgery will eliminate the pain but the process that caused the pain will continue without the use of orthotics. If orthotics have been prescribed prior to surgery they generally do not have to be remade.
Why do I have pain in my heel?
Prevention

Wear shoes that fit well, front, back and sides and have shock-absorbent soles, rigid uppers and supportive heel counters. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm-up before running or walking, and do some stretching exercises afterward. Pace yourself when you participate in athletic activities. If overweight, try non weight-bearing activities such as swimming or cycling. Your podiatrist may also use taping or strapping to provide extra support for your foot. Orthoses (shoe inserts) specifically made to suit your needs may be also be prescribed.
How You Can Fix Functional Leg Length Discrepancy
Approximately 75% of us present with one leg longer than the other. It?s staggering, literally, that so many people walk about with an imbalance. Yet to have one leg longer than the other doesn?t seem to create pain for everyone but for those that it does it brings pain in a myriad of dysfunction from TMJ, headaches, low back pain, IBS, bladder problems, sexual dysfunction, sacroiliac joint pain, pubis dysfunction, groin strain, gluteal dysfunction as well as the formation of trigger points.

Causes
There are many causes of leg length discrepancy. Some include, A broken leg bone may lead to a leg length discrepancy if it heals in a shortened position. This is more likely if the bone was broken in many pieces. It also is more likely if skin and muscle tissue around the bone were severely injured and exposed, as in an open fracture. Broken bones in children sometimes grow faster for several years after healing, causing the injured bone to become longer. A break in a child's bone through the growth center near the end of the bone may cause slower growth, resulting in a shorter leg. Bone infections that occur in children while they are growing may cause a significant leg length discrepancy. This is especially true if the infection happens in infancy. Inflammation of joints during growth may cause unequal leg length. One example is juvenile arthritis. Bone diseases may cause leg length discrepancy, as well. Examples are, Neurofibromatosis, Multiple hereditary exostoses, Ollier disease. Other causes include inflammation (arthritis) and neurologic conditions. Sometimes the cause of leg length discrepancy is unknown, particularly in cases involving underdevelopment of the inner or outer side of the leg, or partial overgrowth of one side of the body. These conditions are usually present at birth, but the leg length difference may be too small to be detected. As the child grows, the leg length discrepancy increases and becomes more noticeable. In underdevelopment, one of the two bones between the knee and the ankle is abnormally short. There also may be related foot or knee problems. Hemihypertrophy (one side too big) or hemiatrophy (one side too small) are rare leg length discrepancy conditions. In these conditions, the arm and leg on one side of the body are either longer or shorter than the arm and leg on the other side of the body. There may also be a difference between the two sides of the face. Sometimes no cause can be found. This is known as an "idiopathic" difference.
Symptoms
The effects vary from patient to patient, depending on the cause of the discrepancy and the magnitude of the difference. Differences of 3 1/2 to 4 percent of the total length of the lower extremity (4 cm or 1 2/3 inches in an average adult), including the thigh, lower leg and foot, may cause noticeable abnormalities while walking and require more effort to walk. Differences between the lengths of the upper extremities cause few problems unless the difference is so great that it becomes difficult to hold objects or perform chores with both hands. You and your physician can decide what is right for you after discussing the causes, treatment options and risks and benefits of limb lengthening, including no treatment at all. Although an LLD may be detected on a screening examination for curvature of the spine (scoliosis), LLD does not cause scoliosis. There is controversy about the effect of LLD on the spine. Some studies indicate that people with an LLD have a greater incidence of low back pain and an increased susceptibility to injuries, but other studies refute this relationship.
Diagnosis
Infants, children or adolescents suspected of having a limb-length condition should receive an evaluation at the first sign of difficulty in using their arms or legs. In many cases, signs are subtle and only noticeable in certain situations, such as when buying clothing or playing sports. Proper initial assessments by qualified pediatric orthopedic providers can reduce the likelihood of long-term complications and increase the likelihood that less invasive management will be effective. In most cases, very mild limb length discrepancies require no formal treatment at all.
Non Surgical Treatment
Treatment of leg length inequality involves many different approaches, which vary among osteopaths, physiotherapist and chiropractor and whether the LLD is functional or structural. Thus is a combination of myofascial release (massage) & stretching of shortened muscles. Manipulation or mobilization of the spine, sacro-iliac joint (SIJ), hip, knee, foot. Orthotics, shoe lifts can be used to treat discrepancies from two to six cm (usually up to 1 cm can be inserted in the shoe. For larger leg length inequalities, the shoe must be built up. This needs to be done for every shoe worn, thus limiting the type of shoe that the patient can wear). Surgery (epiphysiodesis, epiphyseal stapling,bone resection).

what is a functional leg length discrepancy?
Surgical Treatment
The bone is lengthened by surgically applying an external fixation device to the leg. The external fixator, a scaffold-like frame, is connected to the bone with wires, pins, or both. A small crack is made in the bone and the frame creates tension when the patient or family member turns its dial. This is done several times each day. The lengthening process begins approximately five to 10 days after surgery. The bone may lengthen 1 millimeter per day, or approximately 1 inch per month. Lengthening may be slower in a bone that was previously injured. It may also be slower if the leg was operated on before. Bones in patients with potential blood vessel abnormalities, such as cigarette smokers, may also need to be lengthened more slowly. The external fixator is worn until the bone is strong enough to support the patient safely. This usually takes about three months for each inch. Factors such as age, health, smoking and participation in rehabilitation can affect the amount of time needed.
Treating Mortons Neuroma
 Morton?s neuroma is a swollen nerve in the distal portion of the foot. The enlarged portion of the nerve represents scarring within the plantar nerve that occurs after chronic compression and/or repetitive injury. This may come about when the toes are squeezed together for too long, as can occur with the chronic use of high heels. The nerve that runs between your toes will swell and thicken. This can cause pain when walking. The symptoms of Morton?s neuroma can include burning pain in the foot, the feeling of a lump inside your foot, pain between the third and fourth toes typically but it can occur between other toes.
Morton?s neuroma is a swollen nerve in the distal portion of the foot. The enlarged portion of the nerve represents scarring within the plantar nerve that occurs after chronic compression and/or repetitive injury. This may come about when the toes are squeezed together for too long, as can occur with the chronic use of high heels. The nerve that runs between your toes will swell and thicken. This can cause pain when walking. The symptoms of Morton?s neuroma can include burning pain in the foot, the feeling of a lump inside your foot, pain between the third and fourth toes typically but it can occur between other toes.Causes
Various factors have been implicated in the precipitation of Morton's neuroma. Morton's neuroma is known to develop as a result of chronic nerve stress and irritation, particularly with excessive toe dorsiflexion. Poorly fitting and constricting shoes (ie, small toe box) or shoes with heel lifts often contribute to Morton's neuroma. Women who wear high-heeled shoes for a number of years or men who are required to wear constrictive shoe gear are at risk. A biomechanical theory of causation involves the mechanics of the foot and ankle. For instance, individuals with tight gastrocnemius-soleus muscles or who excessively pronate the foot may compensate by dorsiflexion of the metatarsals subsequently irritating of the interdigital nerve. Certain activities carry increased risk of excessive toe dorsiflexion, such as prolonged walking, running, squatting, and demi-pointe position in ballet.
Symptoms
Pain is usually increased by forefoot weight bearing activities (such as running), with narrow-fitting footwear, or with high heeled shoes. It is usually painful to firmly touch the affected region and, in chronic cases, pain and sometimes an audible click, may be heard when squeezing the foot and toes together with the hand. Often a localized area of swelling may be evident at the site of injury.
Diagnosis
An MRI scan (magnetic resonance imaging) is used to ensure that the compression is not caused by a tumor in the foot. An MRI also determines the size of the neuroma and whether the syndrome should be treated conservatively or aggressively. If surgery is indicated, the podiatrist can determine how much of the nerve must be resected. This is important, because different surgical techniques can be used, depending on the size and the position of the neuroma. Because MRIs are expensive, some insurance companies are reluctant to pay for them. If the podiatrist believes an MRI is necessary, he or she can persuade the insurance company to pay for it by presenting data to support the recommendation.
Non Surgical Treatment
Treatment options vary with the severity of each neuroma, and identifying the neuroma early in its development is important to avoid surgical correction. For simple, undeveloped neuromas, a pair of thick-soled shoes with a wide toe box is often adequate treatment to relieve symptoms, allowing the condition to diminish on its own. For more severe conditions, however, additional treatment or surgery may be necessary to remove the tumor. The primary goal of most early treatment regimens is to relieve pressure on areas where a neuroma develops. Your podiatric physician will examine and likely X-ray the affected area and suggest a treatment plan that best suits your individual case. Padding and Taping. Special padding at the ball of the foot may change the abnormal foot function and relieve the symptoms caused by the neuroma. Medication. Anti-inflammatory drugs and cortisone injections can be prescribed to ease acute pain and inflammation caused by the neuroma. Orthotics. Custom shoe inserts made by your podiatrist may be useful in controlling foot function. Orthotics may reduce symptoms and prevent the worsening of the condition.
Surgical Treatment
If other therapies have not worked it may be necessary to perform surgery. As surgery may result in permanent numbness in the affected toe, doctors ten to use this procedure as a last resort. However, in most cases surgery is extremely effective. The patient usually receives a local anesthetic. Surgery involves either removing the nerve, or removing the pressure on the nerve. Two surgical approaches are possible. The dorsal approach, the surgeon makes an incision on the top of the foot, allowing the patient to walk soon after surgery, because the stitches are not on the weight-bearing side of the foot. The plantar approach, the surgeon makes an incision on the sole of the foot. In most cases the patient will be in crutches for about three weeks. The resulting scar may make walking uncomfortable. However, with this approach the neuroma can be reached easily and resected without cutting any structures. There is a small risk of infection around the toes after surgery.
Hammer Toe Cause & Treatment Solution
 Overview
Overview
hammertoe is a painful deformity wherein a toe bends unnaturally and becomes clawlike. This happens because the tendons of the toe contract abnormally, forcing the toe to bend downward and the middle joint of the toe to protrude upward. Although any toe may be affected, hammertoe usually affects the second toe. The toe assumes a clawlike position and cannot be straightened out. When someone with hammertoe wears shoes, the toe is constantly rubbed, so walking may become especially painful if a callus on the sole of the foot or a corn on the top of a toe develops.
Causes
Wearing ill-fitting shoes is probably the main cause of hammer toe. As the toe bends, tendons add to the problem by contracting in such a way that the bending is reinforced to the point of becoming permanent. In some cases, tendons that are abnormal to begin with may start the bending process.
 Symptoms
Symptoms
The most obvious symptoms of this injury will be the the middle toe joint is permanently bent at an angle. In the beginning movement may still be possible but as time passes and the injury worsens the toe will be locked in place and possible require hammer toe correction surgery to fix. Another key indicator of hammer toe is that a lump or corn will form on top of the toe. The toe joint will be painful and walking can cause severe discomfort. Occasionally a callus may form on the sole of the injured foot. If you see any of these symptoms together or have been enduring pain for some time, seeing a podiatrist should be your next step.
Diagnosis
The treatment options vary with the type and severity of hammertoes each hammer toe, although identifying the deformity early in its development is important to avoid surgery. Your podiatric physician will examine and X-ray the affected area and recommend a treatment plan specific to your condition.
Non Surgical Treatment
Changing the type of footwear worn is a very important step in the treatment of hammer toes. When choosing a shoe, make sure the toe box (toe area) is high and broad, and can accommodate the hammer toes. A shoe with a high, broad toe box will provide enough room in the forefoot area so that there is less friction against the toes. Other conservative treatments include using forefoot products designed to relieve hammer toes, such as hammer toe crests and hammer toe splints. These devices will help hold down the hammer toe and provide relief to the forefoot. Gel toe shields and gel toe caps are also recommended to eliminate friction between the shoe and the toe, while providing comfort and lubrication.
Surgical Treatment
Surgery to correct for a hammertoe may be performed as an outpatient procedure at a hospital, surgery center, or in the office of your podiatrist. There are multiple procedures that can be used depending on your individual foot structure and whether the deformity is flexible or rigid. There may be a surgical cut in the bone to get rid of an exostosis, or a joint may be completely removed to allow the toe to lay straight.
Hammer Toe Symptoms
 Overview
Overview
There are two different types of Hammertoe. Flexible Hammer Toes. These hammer toes are less serious because they can be diagnosed and treated while still in the developmental stage. They are called flexible hammer toes because they are still moveable at the joint. Rigid Hammer Toes. This variety is more developed and more serious than the flexible condition. Rigid hammer toes can be seen in patients with severe arthritis, for example, or in patients who wait too long to seek professional treatment. The tendons in a rigid hammer toe have become tight, and the joint misaligned and immobile, making surgery the usual course of treatment.
Causes
The incorrect position of the person's toes inside of their shoes also causes the formation of calluses or corns on the surfaces of their toes which are constantly bent as they are wearing inappropriate shoes because the surfaces are consistently rubbing against the hard materials of the interior of the shoes causing regular friction. 
Symptoms
Hammer, claw, and mallet toes can cause discomfort and pain and may make it hard to walk. Shoes may rub on your toes, causing pain, blisters, calluses or corns, or sores. Sores can become infected and lead to cellulitis or osteomyelitis, especially if you have diabetes or peripheral arterial disease. If you have one of these health problems and sores develop, contact your doctor.
Diagnosis
Your doctor is very likely to be able to diagnose your hammertoe simply by examining your foot. Even before that, he or she will probably ask about your family and personal medical history and evaluate your gait as you walk and the types of shoes you wear. You'll be asked about your symptoms, when they started and when they occur. You may also be asked to flex your toe so that your doctor can get an idea of your range of motion. He or she may order x-rays in order to better define your deformity.
Non Surgical Treatment
Hammertoes that are not painful (asymptomatic) and still flexible may not require treatment. In mild cases, open-toed, low-heeled, or wider shoes and foam or moleskin pads can provide symptomatic relief by reducing pressure. Taping (strapping) the affected toe can help to reduce deformity and pain. Physical therapy to instruct patients in exercises that passively stretch tight structures and strengthen weak foot intrinsic muscles is also helpful with mild cases. Periodic trimming (debridement) of corns (clavi, helomata) by a podiatrist can provide temporary relief. Corticosteroid injections are often very effective in reducing pain.
Surgical Treatment
Extreme occurrences of hammer toe may call for surgery. Your surgeon will decide which form of surgery will best suit your case. Often, the surgeon may have to cut or remove a tendon or ligament. Depending on the severity of your condition, the bones on both sides of the joint afflicted may need to be fused together. The good news is you can probably have your surgery and be released to go home in one day. You will probably experience some stiffness in your toe, but it might last for a short period, then your long-term pain will be eliminated.
How To Get Rid Of Bunions Naturally
Overview
 Hallux valgus, often referred to as "a bunion," is a deformity of the big toe. The toe tilts over towards the smaller toes and a bony lump appears on the inside of the foot. (A bony lump on the top of the big toe joint is usually due to a different condition, called hallux rigidus.) Sometimes a soft fluid swelling develops over the bony lump. The bony lump is the end of the "knuckle-bone" of the big toe (the first metatarsal bone) which becomes exposed as the toe tilts out of place.
Hallux valgus, often referred to as "a bunion," is a deformity of the big toe. The toe tilts over towards the smaller toes and a bony lump appears on the inside of the foot. (A bony lump on the top of the big toe joint is usually due to a different condition, called hallux rigidus.) Sometimes a soft fluid swelling develops over the bony lump. The bony lump is the end of the "knuckle-bone" of the big toe (the first metatarsal bone) which becomes exposed as the toe tilts out of place.
Causes
No one single cause has been proven. There are a number of causes, and though shoes can exacerbate the problem, bunions do occur in societies that don?t wear them. We walk on the same type of ground all the time, whereas the human foot was actually designed to adapt to varying terrains. In a sense, a bunion is a type of repetitive strain injury. And like repetitive strain injury, some people are more prone to it than others. One theory, though it remains unproven, is that bunions are caused by one or both of the following. Because the foot wasn?t designed to constantly walk on a level surface, the ball of the big toe is slightly lower than the ball of the rest of your foot. When your foot meets the ground, the ball of the big toe is pushed up, and the big toe joint can?t bend as well as it was designed to. In order for the big toe joint to bend fully as you walk, your foot rolls slightly over to the side (this is also why people with hallux valgus often get hard skin). Also, if your midtarsal joint tends to move from side to side more than it does up and down, the arch in your foot collapses as your foot rolls in. This also makes you more prone to developing bunions. Such problems can be exacerbated by tight footwear. Slip-on shoes can make matters worse. Because they have to be tighter to stay on your feet, you automatically have less room for your toes. And with nothing to hold your foot in place, your toes often slide to the end where they?re exposed to lots of pressure. Likewise, high heels throw more weight onto the ball of the foot, putting your toes under further pressure. If you haven?t got a bunion by adulthood and you later develop one, there could be some underlying arthritis.
Symptoms
symptoms and problems caused by bunions include pain. You may then have difficulty walking due to pain. Inflammation and swelling at the base of the toe. This sometimes becomes infected. The foot may become so wide that it can be difficult to find wide enough shoes. You may get arthritis in the big toe. The second toe can become deformed. In severe cases, the big toe can push your second toe up out of place.
Diagnosis
A thorough medical history and physical exam by a physician is necessary for the proper diagnosis of bunions and other foot conditions. X-rays can help confirm the diagnosis by showing the bone displacement, joint swelling, and, in some cases, the overgrowth of bone that characterizes bunions. Doctors also will consider the possibility that the joint pain is caused by or complicated by Arthritis, which causes destruction of the cartilage of the joint. Gout, which causes the accumulation of uric acid crystals in the joint. Tiny fractures of a bone in the foot or stress fractures. Infection. Your doctor may order additional tests to rule out these possibilities.
Non Surgical Treatment
In most cases the symptoms of bunions can be reduced or relieved without surgery. Reducing pressure on the bunion is the first step in reducing the pain associated with the condition. Wearing correctly fitting shoes is important in achieving this. A referral to a podiatrist may be made in order to assess the need for special orthotic devices, such as custom-made arch supports and shoe inserts (eg: metatarsal pad or bar). These can help to relieve tension on the base of the big toe and help prevent flat-footedness. Specific exercises and bunion pads available over-the-counter at pharmacies may also be of benefit. Anti-inflammatory medicines can help to ease pain in the short term. Steroid injections may be used to relieve severe pain. If a sufficient reduction in symptoms is not achieved by non-surgical treatment, then surgery may be recommended. 
Surgical Treatment
Bunion surgery is occasionally required when the bunion deformity is too advanced for conservative treatment to work. Your surgeon will usually cut an angular section from the bone to correct the alignment. In some cases, multiple toes may need to be straighten.